What Is Known: The True Cause of Eczema
Healthy Steps: Eczema—First Steps
Healthy Steps: Eczema—Full Program
Preventing Eczema
From Dr. Deborah's Desk
Updated December 8, 2012
Scratch, scratch, "don't scratch!"
If you've ever wished you could unzip from your old skin and step into a brand-new epidermis for one night just so you could get some sleep, you are probably all too familiar with the itchy, bumpy, blistery, crackling rash known as eczema. While you can't make like a snake and shed your existing skin, there are some simple steps you can take to naturally treat the eczema, alleviating the problem from the inside out.
What Is Known: The True Cause of Eczema
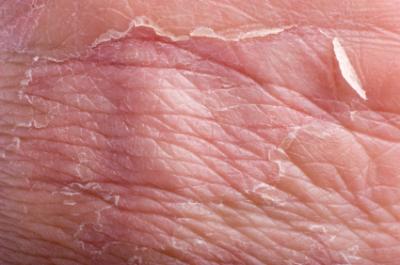
Eczema is an inflammatory skin condition often referred to as atopic dermatitis. Symptoms may include red, inflamed, itchy, bumpy, blistery, toughened, and cracking chronic skin eruptions. Many cases of eczema reflect an allergic type sensitivity to a food taken internally, a product applied externally, an environmental allergen, a drying or irritating agent, or a laundry detergent. Like hives, eczema may be associated with reduced stomach acid. In some people, stress or temperature extremes can cause eczema to flare. All of these “causes” are worth investigating because if a true stimulus can be eliminated, the eczema can be easily resolved.
Conventional medical treatments such as steroid creams block the body's inflammatory response without eliminating the cause of the eczema, merely masking the symptoms and often worsening the condition.
For example, an interesting observation from homeopathic experience reveals that eczema is sometimes the temporary result of a cleansing or purging of toxins from the body, occurring during the relief of a more serious underlying medical condition. Natural and gentle topical treatments can help minimize the discomfort of the rash without interfering with the deeper healing taking place inside the body. By contrast, overly aggressive treatments (e.g., cortisone suppression of all eczematous lesions) actually suppress the release of the toxins, often resulting in a return of the original and more serious medical problems that preceded the eczema.
By reducing the inflammation through lifestyle choices, nutrition, and supplements, you can better equip your body to lessen the severity and frequency of eruptions.
Healthy Steps: Eczema—First Steps
For the greatest improvement with the fewest steps, do the following:
- Eat Omega-3 fats, best for you in:
- Barleans Fish Oil: 1 tablespoon daily with food
- Grass-fed meats, wild Alaskan salmon and halibut, herring, oysters, and sardines
- Stop all grains (except rice) for 6 weeks.
- Use Calendula ointment. Naturally soothing to the skin. For more intense treatment use Aim2Health Double Strength TheraCream with urea to relieve itching and heal lesions.
Healthy Steps: Eczema—Full Program
Follow our basic nutrition and healthy lifestyle guidelines, with the following modifications:
Savor Helpful Foods
- Coconut oil: 3 tablespoons daily with cooking or raw in smoothies.
- Omega-3 fats, preferably as they occur naturally in grass-fed meats, wild Alaskan salmon and halibut, herring, oysters, and sardines.
- Salmon caviar (a.k.a. fish roe): 1-3 roe daily
- Nuts, particularly walnut. Prepare them as Crispy Nuts. Peanuts are legumes, not nuts.
- Dark, leafy greens - such as collards, dandelion, kale, nettles, and plantain - cooked, with lots of butter.
- Vegetable juices. Any combination of leafy greens, a little bit of beet, bell pepper, cabbage, carrot, celery, chickweed, cilantro, clover, cucumber, and zucchini will be delicious and nutritious.
- Oolong tea, midway in the fermentation between green and black tea, has reduced eczema in doses of 100 mg daily.
- For infants: Breastfeeding for a minimum of six months. Breastfeeding newborns for a minimum of 6 months (longer is better) is recommended to reduce the risk of eczema as well as a host of viral and bacterial infections.
Avoid Common Allergens or Irritants for 6-12 Weeks:
- Grains: Common offenders are corn and all gluten-containing grains (barley, rye, wheat and beer). Gluten is linked to a specific skin rash (dermatitis herpetiformis) in people with celiac disease and may aggravate eczema even in non-celiac patients. For any child, withhold all grains until one year old, then start them one at a time and always soaked and sprouted. Save wheat for last and consider not giving wheat at all.
- Proteins such as beef, chicken, eggs, pork, and seafood: Start by eliminating all of these for one week and substitute with game meats such as turkey, bison, and elk. As a crucial food group, protein cannot simply be eliminated or restricted to just turkey, so after the first week, add back in one of the food types each week. Save eggs, sadly, for last, as they are a common allergen.
- Omega 6 fatty acids: I often tell patients that the least expensive way to take omega-3 fatty acids is to eliminate excess sources of omega-6 fatty acids. Some omega-6's naturally occur in meat, nuts, and vegetables, but by far the greatest sources in the typical diet are processed foods, particularly pre-made salad dressings. Every pre-made dressing has excessive omega 6's (whatever it says on the front), and you can make your own with olive oil and vinegar!
- Citrus fruits and strawberries.
- Pasteurized dairy products: Milk allergy is a frequently cited cause of eczema and other allergic conditions. At least one study, however, has shown that raw milk consumption is associated with a significantly reduced risk of asthma. Other studies have credited raw milk with reduction of allergies and asthma, conditions closely associated with eczema. We recommend avoiding all dairy products for 4-6 weeks. Thereafter, include raw, whole-fat dairy in small amounts while continuing to avoid pasteurized dairy products.
- Processed foods.
- Trans fats: Fats and fatty acids play a crucial role in skin health, but all synthetic, altered fats should be avoided.
- Tomatoes.
- White potatoes.
- Soy and soy-based products.
- All legumes with the exception of black beans. Remember that peanuts are legumes!
- Unnecessary medications: Many chemicals and drugs (over-the-counter and prescription) can trigger eczema to the extent that they are disrupting agents for an individual's physiology. Continue all medications prescribed by your doctor and find natural alternatives for medications you have chosen for yourself. As your health improves, you may be able to consult with your physician about reducing one or more of your prescription medications.
- Alcohol, chocolate, sugar, yeast, coffee, and black tea (except oolong tea).
Supplements Can Help:
- Barlean's Fish Oil: 1 tablespoon daily.
- Probiotics: Allergy Research Group Synbiotics with FOS Powder, start with 1/4 tsp daily and build as tolerated, to 1/2 Tbsp daily. Alternatively, seek other broad-spectrum probiotics.
- Pure Encapsulations Evening Primrose Oil: Take 2-12 capsules (500 mg each) daily.
- Biotics Research Bio-D-Mulsion Forte 2000iu: Individual vitamin D3 doses should adjusted to maintain a D3 blood level (25(OH)D test) of 40-65 ng/ml. Adults usually require 2,000-6,000 IU, and children 10-25 IU per pound. Recheck after three to six months. D3 should be taken with a meal that includes healthy fats (preferably animal fats) for best absorption.
- Thorne Research Magnesium Citramate: Take 150-600 mg daily or to bowel tolerance.
- Thorne Research DiPan-9: Take 1-3 capsules with each meal.
- Thorne Research Zinc Picolinate: (15-30 mg) 1-3 times daily for 6-12 weeks, then reduce to once daily (NOTE: high dose zinc supplementation should always be balanced with adequate copper intake)
- Thorne Research Betaine HCl: Take 1-3 capsules with each meal as a therapeutic trial for two weeks. One of the causes of eczema can be low levels of stomach acid.
Topical treatments try any of these for relief:
- Expose your skin to the sun without burning. Gradually increase to 20 minutes daily, full body if possible! The sun provides our best source of vitamin D and is very healing for eczema. Best time is between 11-2 in the summer.
- Dr. Bronners - Magic Fresh-Pressed Virgin Coconut Oil, applied topically. A mild antibacterial and antiviral moisturizer, apply daily after bathing or showering. The same oil used for cooking works fine. Any virgin coconut oil will work, but Dr. Bronner's is the easiest to rub into your skin.
- Honey (raw and local preferred) or liquid vitamin E. Apply directly to cracked skin as a natural wound dressing.
- Calendula ointment. Naturally soothing to the skin. For more intense treatment use Aim 2 Health Double Strength TheraCream. Urea skin cream applied topically increases moisture in the skin by enhancing the water-binding capacity of skin cells. Although it may cause temporary minor stinging, urea is non-irritating and has a rapid calming effect on inflamed, itchy skin rashes. It also helps to prevent infection and heals wounds without scarring. Follow the directions on the label for coverage and frequency of application.
- Saltwater compresses relieve itching and soothe irritated skin. For the compress, mix high quality celtic sea salt with warm filtered water (1:2 ratio) and soak a clean washcloth until saturated, then apply to skin.
- Oatmeal baths. Grind two cups of dry rolled oats to a fine powder and place in a cheesecloth sack. Add the sack to a tepid bath. Soak for 15 minutes, then pat skin dry without rinsing.
- Herb Pharm Original Salve is a beeswax based salve is available through my office, or you can make your own. Mix beeswax and a gentle oil (olive or almond) with calendula, comfrey, goldenseal, or other healing herbs. A thin coat of salve applied 1-4 times daily can be very soothing.
Caution: Cortisone in eczema creams, whether “natural”, over the counter, or by prescription, may be used carefully to reduce suffering without compromising the internal healing that is of primary importance. Hydrocortisone cream, 1-2%, mixed with an herbal calendula-containing salve or ointment, can soothe the angriest (or most visible!) lesions. Applying it to widely can result in two potential problems: first, the suppression of the eczema without a true healing, and secondly, the patient will often develop a tolerance to steroid creams, eventually requiring increased or fluorinated (skin damaging) doses.
Other Irritants to Avoid:
- Scratching the itch. This is probably the number one cause of worsening eczema. Please do all that you can to avoid scratching including wearing white cotton gloves while you sleep. This can be especially helpful for children.
- Fluoride in toothpaste may affect facial eczema.
- Excess (frequent or overly hot) bathing and chlorine. Limit bathing. Overly frequent bathing or use of too-hot water or chlorine can aggravate eczema. Children often do fine with weekly immersion baths or showers, and adults rarely need daily bathing unless they are very physically active. Supplement with daily spot sponge baths. Where whole house filtration is not possible as a means of removing chlorine, use a simple filter for the bath or shower. For more information about the effects of chlorine and our recommended water filtration methods, read our article Water and Walter Filters and Chlorine in Our Water.
- Commercially manufactured antibacterial soap. Avoid excessively drying the skin; use soap only where necessary and minimize the frequency of baths and showers. Avoid antibacterial soaps and use simple natural moisturizing soaps instead. Even if eczema is “open,” antibacterial soaps are excessively harsh. Where soap is necessary, select a very mild oil-based (coconut, neem, olive, etc.) soap.
- Synthetic ingredients such as parabens, mineral oil, paraffin, petroleum, sodium lauryl sulfates, acrylamide, propylene glycol, pheonol carbolic acid, dioxan, and toluene.
Homeopathic Treatment
I recommend against any non-professional use of homeopathic remedies for eczema. If you wish to be treated homeopathically I can help you find a professional homeopath in your area.
Prevention: What Can You Do?
Identifying the cause of your eczema is important to both resolving and preventing the condition. Whether your own eczema is triggered by internal factors such as food allergies, reduced stomach acid, or stress or external factors such as body products, heat, laundry detergents, household cleaning products, or fibrous materials like wool, eliminating the stimulus is the key to resolving your eczema.
My approach focuses on reducing inflammation through lifestyle, nutrition, natural topical treatments, and supplements. All of these work in conjunction with each other to help your body heal on the inside while calming the skin on the outside. This method results in less frequent and milder eruptions, while simultaneously supporting the body in healing the root cause of the condition.
From Dr. Deborah's Desk
Isn't it amazing how many different factors can affect eczema? Eczema is actually a perfect example of the canary in the coal mine: silent canaries were a warning to the miners that they were in danger from low oxygen, and eczema is your body's warning sign about danger from excess inflammation. So while the Healthy Steps comprise a very long list, every step you take to calm your eczema can reduce your body's load of inflammation and reduce your risk of other chronic diseases. Start with a few steps, and add others as needed.
In my experience, the place to start is to identify potential allergens, and a great way to do that is to eliminate grains and sugars from your diet. For many people that is enough. Period.
For more serious cases, add the First Steps supplements, and revise your bathing routine. No chlorine or harsh soaps, less frequent bathing, and always follow bathing with a gentle moisturizer. My favorite is coconut oil.
Stress is blamed for everything, but it's not a cause for everyone, is it true for you? I'm looking forward to including many techniques I've learned from my experience and my patients in our developing Mind, Body and Soul section. For today, write your own doctor's prescription: what would lighten your mood right now? Plan your first Healthy Steps then take a break and follow your own prescription.
This information is provided for educational purposes only, and any individual diagnosis or treatment should be determined by you and your doctor. See Additional Information for more details.
